You may not be demobilized, but you feel disturbing pain sensations while walking, standing or sitting. A sensation like tingling pain from your back through to the buttocks, thighs, feet and toes; then, you might be experiencing sciatica. Any form of pain is bad enough for daily activities. It, however, becomes worse and alter lifestyles when mobility parts like back, legs and feet are directly affected. Pain in mobility parts of the body can stop you from doing all of the things you love, as well as have a bad effect on your mental health.
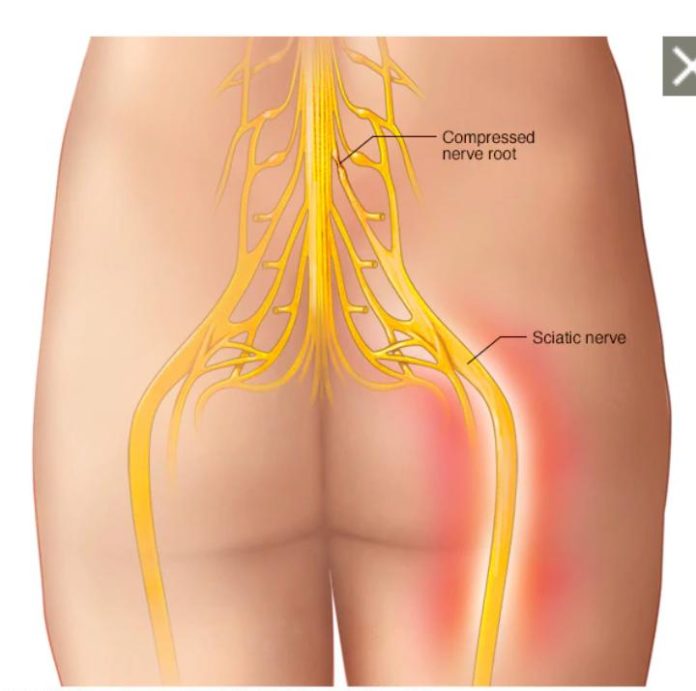
Sciatica is a type of pain that stems from the inflammation of the sciatic nerve. This nerve carries messages from your brain, all the way down your back (spinal cord) to your legs and feet. Normally, one of the signs of sciatica is pain that radiates down one side of your body, starting at the lower back and running down the leg to just below the knee. It can also cause muscle weakness and numbness in the legs.
Usually, sciatica affects only one leg at a time and the symptoms radiate from the lower back or buttock to the thigh and down the leg. Sciatica may cause pain in the front, back, and/or sides of the thigh and leg. But in some rare cases sciatica can affect the two legs at a time particularly if the cause is as a result of degenerative disk.
Symptoms
Sciatica pain may be constant or intermittent. The pain is usually described as a burning sensation or a sharp, shooting pain. The pain is usually more severe in the leg compared to the back. Leg pain commonly occurs more in the calf region below the knee compared to other parts of the leg.
– Altered sensation. Numbness, tingling, and/or a pins-and-needles sensation may be felt at the back of the leg.
–Weakness. Weakness may be felt in the leg and foot. A feeling of heaviness in the affected leg may make it difficult to lift the foot off the floor.
-Change in posture may aggravate or relieve pain. Certain postures may affect sciatica pain: Sciatica pain may feel worse while sitting, trying to stand up, standing for a long time, bending the spine forward, twisting the spine, and/or while coughing.
Pain may increase or remain constant while lying down, causing disturbed sleep. Lying on the back with the knees slightly elevated and propped up with a pillow, or lying on the side with a pillow between the legs, may help relieve the pain in such cases.
The pain may be relieved while walking, applying a heat pack to the rear pelvic area, or doing pelvic exercises. Other symptoms include:
- Lower back pain
- Pain in the rear or leg that is worse when sitting
- Hip pain
- Burning or tingling down the leg
- Weakness, numbness, or a hard time moving the leg or foot
- A constant pain on one side of the rear
- A shooting pain that makes it hard to stand up
Sciatica usually affects only one side of the lower body. Often, the pain extends from the lower back all the way through the back of your thigh and down through your leg. Depending on where the sciatic nerve is affected, the pain may also extend to the foot or toes.
For some people, the pain from sciatica can be severe and disabling. For others, the sciatica pain might be infrequent and irritating, but has the potential to get worse.
Seek medical attention right away if you have:
- Fever and back pain
- Swelling or redness in your back or spine
- Pain that moves down your legs
- Numbness or weakness in the upper thighs, legs, pelvis, or bottom
- Burning when you pee or blood in your pee
- Serious pain
- Loss of bladder or bowel control (leaking or not being able to make it to the toilet in time)
Common causes of sciatica and Risk Factors include:
- Lumbar spinal stenosis (narrowing of the spinal canal in your lower back)
- Degenerative disk disease (breakdown of disks, which act as cushions between the vertebrae)
- Spondylolisthesis (a condition in which one vertebra slips forward over another one)
- Pregnancy
- Muscle spasm in the back or buttocks
Other things that may make you more likely to have sciatica include:
- Aging (which can cause changes in the spine, like bone spurs or herniated disks)
- Diabetes
- Being overweight
- Not exercising regularly
- Wearing high heels
- Sleeping on a mattress that is too hard or too soft
- Smoking
- Your job, especially if it involves driving for long periods of time, twisting your back, or carrying heavy things
Types
Depending on the duration of symptoms and if one or both legs are affected, sciatica can be of different types:
–Acute sciatica. Acute sciatica is a recent onset, 4 to 8-week duration of sciatic nerve pain. The pain may be self-managed and may not typically require medical treatment.
–Chronic sciatica. Chronic sciatica is persistent sciatic nerve pain that lasts for more than 8 weeks and usually does not subside with self-management. Depending on the cause, chronic sciatica may require nonsurgical or surgical treatment.
–Alternating sciatica. Alternating sciatica is sciatic nerve pain that affects both legs alternately. This type of sciatica is rare and may result from degenerative problems in the sacroiliac joint.
–Bilateral sciatica. Bilateral sciatica occurs in both legs together. This type of sciatica is rare and may occur due to degenerative changes in the vertebrae and/or the disc at several spinal levels.
– Wallet sciatica: sciatic pain that occurs while sitting on a wallet (or any object in the back pocket of a trouser).
Diagnosis & Treatment
Although sciatica can be extremely painful, it is very rarely harmful. For most people suffering from sciatica, symptoms generally improve over a few weeks with conservative treatment. There are other options such as spinal injections, which can give immediate relief to very bad pain.
If your doctor thinks you have sciatica, you’ll get a physical examination so they can check your reflexes and see how strong your muscles are. They might have you do certain activities, like walking on your heels or toes, to see what’s causing your pain.
If your pain is severe, the doctor might order imaging tests like X-Ray, CT scan, MRI EMG etc. to check for bone spurs and herniated disks. You could get tests like:
Most people with sciatica feel better after self-care activities or at-home remedies like:
- Using cold or hot packs
- Stretching
- Over-the-counter pain medication
But if your pain isn’t getting better, your doctor might suggest other options.
Medication: Anti-inflammatories, anti-seizures, muscle relaxants, narcotics and anti-depressants. See your doctor for the best medication for you.
A physical therapist can show you how to do exercises that will improve your posture and make you more flexible. They’ll also make the muscles that support your back stronger.
Steroid injections
Your doctor might recommend you get steroid injections shot. They’ll give you a shot that has medicine to help with inflammation around the nerve, which can help reduce your pain. The effects usually last a few months, but they’ll wear off over time.
Surgery
If you have extreme pain that doesn’t get better, weakness, or a loss of bladder or bowel control, your doctor might recommend surgery. They’ll take out the bone spur or herniated disk that’s pressing on your nerves and causing your pain.
Prevention
Sciatica once it started comes and go, so it may not be easy to completely prevent it. We can reduce sciatica problems if we consciously protect our back via:
-Regular exercise. To keep back and core muscle for posture and alignment strong
-Maintain proper posture when you sit. Use seat with good lower back support, armrests and a swivel base. You can place a pillow or rolled towel in the small of the back to maintain normal curve. Keep your kneels and hips level
-Use good body mechanics. if you stand for long periods, rest one foot on a stool or small box from time to time. When you lift something heavy, let your lower extremities do the work. Move straight up and down. Keep your back straight and bend only at the knees. Avoid lifting and twisting simultaneously.


Exercise is very important here, and one might need to get an orthopaedic mattress, to keep the body in shape and guide against back pain.
This is an ailment suffered by many and which we mostly attribute to aging. Sadly,medical care especially physiotherapy is not within the reach of many and,mostly, not sought after.
This awakening is priceless.
Thank you so much for these enlightenment. A lot of people suffer different body pains , from joints to neck, back and different types of pains.
For me, the issue i have is hand pains. I have this severe hand/wrist pains when i turn my hands. I have been to the hospital, did physio, took different nerve relief medications but up till now, i still have pains. The pain comes from wrist /hand to my chest. Please, what can i call this and what should i do? My doctor couldn’t even understand it because normal pain should come from the back to other parts of the body.
I really appreciate your efforts.
Thank you for your comments and sorry for the pains in your hand. our sincere advise is to see an orthopedic physician to do physical examination on the hand.
Hi, i think that i saw you visited my blog thus i came to “return the favor”.I am trying to find things to
enhance my site!I suppose its ok to use some of your ideas!!
0mniartist asmr
Hi my loved one! I wish to say that this post is awesome, great written and come with approximately all
vital infos. I would like to see extra posts like this .
0mniartist asmr
Have you ever considered creating an ebook or guest authoring
on other sites? I have a blog based on the same subjects
you discuss and would really like to have you share some stories/information. I know
my visitors would value your work. If you are even remotely interested,
feel free to send me an e mail. 0mniartist asmr
My brother recommended I might like this web site.
He was totally right. This post actually made my day. You cann’t imagine simply how much time I had spent
for this information! Thanks! 0mniartist asmr
I like the valuable information you provide in your articles.
I’ll bookmark your blog and check again here frequently.
I am quite sure I’ll learn many new stuff right here!
Best of luck for the next! 0mniartist asmr
Wonderful goods from you, man. I’ve have in mind your stuff prior to and you are
simply too great. I really like what you’ve obtained right here, certainly like what you are
saying and the way in which you assert it. You’re making it
enjoyable and you continue to care for to keep it wise. I cant
wait to learn much more from you. This is actually a great
web site. 0mniartist asmr
First off I want to say great blog! I had a quick question in which I’d like to ask if you do not mind.
I was interested to find out how you center yourself and clear your head prior to writing.
I’ve had a tough time clearing my mind in getting my thoughts out there.
I do enjoy writing however it just seems like the first 10 to 15 minutes are usually lost
just trying to figure out how to begin. Any ideas or tips?
Cheers!
This article presents clear idea in favor of the new people of blogging, that in fact how to do blogging.
Pretty section of content. I just stumbled upon your weblog and in accession capital to assert that I get in fact enjoyed account your
blog posts. Any way I’ll be subscribing to your augment and even I achievement you access consistently fast.
magnificent issues altogether, you simply gained a new reader.
What may you suggest about your put up that you simply made a few days in the past?
Any certain?
scoliosis
When I originally commented I clicked the “Notify me when new comments are added” checkbox and now each time a comment is added I get three e-mails with the same comment.
Is there any way you can remove people from that service?
Bless you! scoliosis
scoliosis
What i don’t understood is in fact how you are now not
really much more smartly-preferred than you may be right now.
You’re so intelligent. You know thus considerably with regards to this matter, produced me personally believe it from numerous various angles.
Its like women and men don’t seem to be interested except it’s one thing
to accomplish with Lady gaga! Your individual stuffs outstanding.
At all times maintain it up! scoliosis
scoliosis
Have you ever thought about adding a little bit more than just your articles?
I mean, what you say is fundamental and everything. However think of if you added some great pictures or videos to give your posts more, “pop”!
Your content is excellent but with images and video clips,
this site could undeniably be one of the most beneficial in its niche.
Very good blog! scoliosis
free dating sites
Good day! I could have sworn I’ve visited this web site before but after browsing through many of the posts I
realized it’s new to me. Anyhow, I’m definitely delighted
I found it and I’ll be book-marking it and checking back often! dating sites https://785days.tumblr.com/
dating sites
I am really glad to glance at this website posts which carries tons of
useful data, thanks for providing these kinds of information. dating sites
This piece of writing provides clear idea for the new visitors of blogging, that
really how to do running a blog.
Ahaa, its fastidious dialogue on the topic of this post at this place at
this website, I have read all that, so at this time me also commenting at this place.
Hi there, after reading this awesome piece of writing
i am also glad to share my familiarity here with friends.
Hi there, just became aware of your blog through Google, and found that it’s
truly informative. I am gonna watch out for brussels.
I will appreciate if you continue this in future.
Numerous people will be benefited from your writing.
Cheers!
What i do not realize is in reality how you’re now not really
a lot more well-preferred than you might be right now.
You are so intelligent. You know thus considerably on the subject of this topic, produced me in my opinion believe it from numerous varied angles.
Its like men and women are not fascinated unless it’s one thing to do with
Girl gaga! Your own stuffs nice. At all times take care of it up!
What’s up friends, its wonderful article on the topic of educationand entirely defined, keep it up all the time.
WOW just what I was searching for. Came here by searching
for it
Greetings! Very helpful advice in this particular article! It is the little changes
which will make the biggest changes. Many thanks for
sharing!
I have been exploring for a little bit for any high-quality articles or blog posts
in this kind of area . Exploring in Yahoo I ultimately
stumbled upon this web site. Studying this information So i am happy to
convey that I have a very just right uncanny feeling I came upon exactly what I needed.
I most indubitably will make sure to don?t put out
of your mind this site and give it a look regularly.
Best view i have ever seen !
magnificent post, very informative. I wonder why the other experts of this sector do not notice this. You should continue your writing. I’m confident, you’ve a huge readers’ base already!
I’m really impressed with your writing skills and also with the layout on your
weblog. Is this a paid theme or did you modify it yourself?
Either way keep up the nice quality writing, it is rare to see a great blog like this
one nowadays.
I’m very happy to discover this page. I wanted to thank you for your time for this particularly fantastic
read!! I definitely enjoyed every part of it and i also have you bookmarked to check out new information in your site.
I’m not sure exactly why but this site is loading extremely slow for me.
Is anyone else having this issue or is it a problem on my end?
I’ll check back later and see if the problem still exists.
Best view i have ever seen !